Extended Wear Contacts – Gambling With Your Eyes
Extended Wear is defined as overnight use. Typical extended wear ranges from a few nights a week to up to 30 days of continuous wear. No one can argue that the longer you keep a contact on your eye, the greater the chance for problems to occur. Sleeping in your contacts puts you in the HIGHEST RISK group amongst contact lens wearers. Sleeping in contacts is gambling with your eyes. Two minor problems that frequently occur are red, irritated eyes and blurry vision. Two major problems with serious complications are corneal inflammatory events and ulcerative keratitis (see picture below). The articles found at the end of this post may be used to help prove the reality of the situation.
ranges from a few nights a week to up to 30 days of continuous wear. No one can argue that the longer you keep a contact on your eye, the greater the chance for problems to occur. Sleeping in your contacts puts you in the HIGHEST RISK group amongst contact lens wearers. Sleeping in contacts is gambling with your eyes. Two minor problems that frequently occur are red, irritated eyes and blurry vision. Two major problems with serious complications are corneal inflammatory events and ulcerative keratitis (see picture below). The articles found at the end of this post may be used to help prove the reality of the situation.
But first, here is what makes sense to me.
Contacts by design are porous. They are designed to act like a sponge, allowing them to hold water so they stay comfortable. This design also helps vital elements of our tears, such as oxygen, to pass through. Unfortunately, this design also makes them the perfect place for harmful bacteria to grow and for irritating debris to deposit. Fortunately our eye is designed to withstand these assaults.
Our eyes have many protective features, but one critical feature is our ability to blink. However this blink is only effective while ours eyes are open. A blink will gather then remove potentially irritating and/or harmful debris from the corneas surface. Think of the blink as how a win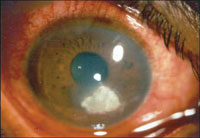 dow washer’s squeegee removes dirt from a window. When we are sleeping, we do not blink. Our eye losses one of its defensive mechanisms and thusly is left in a slightly compromised state. Now picture that dirty, never been cleaned, up to 30 day old contact just sitting on an eye incapable of removing the debris and bacteria from its surface. Its a veritable cesspool. You have the perfect situation for something bad to occur. Overnight wears means a compromised eye subjected to prolonged exposure to debris and bacteria. Now multiply that risk factor by frequency and duration. Are you willing to keep putting your eyes at risk night after night, year after year? Do you really still feel like gambling with the only two eyes you will ever be given? Do you still feel like extended wear conditions will keep your eyes the healthiest? Try a more convenient lens, something that you can take out of you eye and just throw on the floor no matter how tired you are. I would love to save you from a trip to the bathroom to “take out your contacts”(what are the chances you do the best job rubbing, rinsing and soaking them when your in that mood?). Please let me tell you about daily disposables or other healthier ways to wear contacts. Stop sleeping in the lenses. Now.
dow washer’s squeegee removes dirt from a window. When we are sleeping, we do not blink. Our eye losses one of its defensive mechanisms and thusly is left in a slightly compromised state. Now picture that dirty, never been cleaned, up to 30 day old contact just sitting on an eye incapable of removing the debris and bacteria from its surface. Its a veritable cesspool. You have the perfect situation for something bad to occur. Overnight wears means a compromised eye subjected to prolonged exposure to debris and bacteria. Now multiply that risk factor by frequency and duration. Are you willing to keep putting your eyes at risk night after night, year after year? Do you really still feel like gambling with the only two eyes you will ever be given? Do you still feel like extended wear conditions will keep your eyes the healthiest? Try a more convenient lens, something that you can take out of you eye and just throw on the floor no matter how tired you are. I would love to save you from a trip to the bathroom to “take out your contacts”(what are the chances you do the best job rubbing, rinsing and soaking them when your in that mood?). Please let me tell you about daily disposables or other healthier ways to wear contacts. Stop sleeping in the lenses. Now.
RELATED SCIENTIFIC ARTICLES:
Incidence of keratitis of varying severity among contact lens wearers
Aim: To determine the incidence of non-severe keratitis (NSK) and severe keratitis (SK) among wearers of current generation contact lenses.
Methods: A 12 month, prospective, hospital based epidemiological study was conducted by examining all contact lens wearers presenting with a corneal infiltrate/ulcer to a hospital centre in Manchester. A clinical severity matrix was used to differentiate between NSK and SK, based on the severity of signs and symptoms. The size of the hospital catchment population and the wearing modalities (daily wear (DW) or extended wear (EW)) and lens types being used were estimated from relevant demographic and market data.
Conclusions: A clinical severity matrix has considerable utility in assessing contact lens related keratitis. There is a significantly higher incidence of SK in wearers who sleep in contact lenses compared with those who only use lenses during the waking hours.
SOURCE: (2005) Incidence of keratitis of varying severity among contact lens wearers. British Journal of Ophthalmology 89(4):pp. 430-436.
Corneal Inflammatory Events with Extended Contact Lens Wear
High-Dk silicone hydrogel (SH) lenses have been shown to significantly decrease the risk of hypoxic complications compared to traditional low-Dk hydrogels. However, the risks of inflammatory complications with SH compared to that of low-Dk lenses are not as clear. A meta-analysis was performed to combine the relevant literature to evaluate the risks of corneal inflammatory events in users of SH and low-Dk hydrogel extended wear lenses. A systematic search was conducted using online databases, unpublished meeting abstracts and retrieval of other cited references presented or published between 1990 and February 2006. Each study was evaluated for quality in terms of the research question, and these quality assessments were used to determine which studies should be used in subgroup analyses.
Twenty-three studies published or presented on either or both arms by February 2006 were selected for analysis. A total of 9,336 subjects and 18,537 eyes comprised the entire sample. Seven studies were published in the 1990s. Eighteen studies (78 percent) were prospective and 11 (48 percent) used randomization. The follow-up ranged from 4 to 36 months, with a median of 12 months. The rates of infiltrates for low-Dk hydrogels and SH lenses were 7.7 and 14.4 per 100 eye-years, respectively. In the subset of five best quality studies, the unadjusted risk ratio for corneal inflammatory events for SH lenses compared to low-Dk lenses was 2.18. Across studies, adjusted risk ratios ranged from 2.18 to 2.23, with strong confounding between material and length of wear.
Based on published or presented studies between 1991 and 2006, there is approximately a twofold higher risk for corneal inflammatory events in users of SH lenses when typically worn for up to 30 days extended wear when compared with low-Dk extended wear lenses when typically worn for seven days extended wear. The increased risk cannot be definitively linked to SH lens materials because the effect of material on outcome is confounded by length of wear.
SOURCE: Szczotka-Flynn L, Diaz M. Risk of corneal inflammatory events with silicone hydrogel and low dk hydrogel extended contact lens wear: a meta-analysis. Optom Vis Sci 2007;84(4):247-56.
Incidence of Ulcerative Keratitis in Soft Contact Lens Wearers – Extended vs Daily Wear
-
A case-control study of ulcerative keratitis in soft contact lens (CL) users compared three groups of daily wear or extended wear patients: (a) 86 patients with ulcerative keratitis, (b) 61 hospital-based controls, and (c) 410 population-based controls. Overnight lens use, whether regularly with extended wear lenses or occasionally with daily wear lenses, emerged as the preeminent risk factor for ulcerative keratitis. It increased risk by 10 to 15 times in users of extended wear lenses and by 9 times in users of daily wear lenses when these groups were compared with subjects engaged in strict daily wear of daily wear lenses. Even when actual overnight wear was not taken into account, the relative risk was four times greater in users of extended wear lenses than in users of daily wear lenses. The study found a marginal association (p = 0.056) between lens care frequency in general and ulcerative keratitis in comparing ulcerative keratitis cases with population controls. Of the individual hygiene-related measures, evidence of a protective effect was strongest for cleaning the lens case. Smokers showed a threefold greater risk than nonsmokers, regardless of the type of lens worn. An incidence study found the rate of ulcerative keratitis to be approximately 1 in 2,500 daily wear lens users and 1 in 500 extended wear lens users per year. This finding was statistically consistent with the risk ratio noted in the case-control study. Extrapolations suggest that 4,000 of the 9 million U.S. users of daily wear soft lenses develop ulcerative keratitis annually. Among the 4 million U.S. extended wear soft lens users, 8,000 may do so per year.
SOURCE: ScheinOD, Poggio EC Ulcerative keratitis in contact lens wearers. Incidence and risk factors. Cornea. 1990;9 Suppl 1:S55-8; Massachusetts Eye and Ear Infirmary, Department of Ophthalmology, Harvard Medical School, Boston 02114.
-




More people need to read this , because I know a lot of people who SLEEP in their contacts and tell me they are extended , well so are mine but I still take them out every night because I value my eyesight.
02/11/2009 at 1:28 PM